
Understanding Insurance Billing for Teletherapy
Understanding Insurance & Billing for Teletherapy
At Kirkland EMDR Counseling we strive to make the billing process as transparent as possible. We believe in client education and knowing how your insurance works so it’s not a mystery. If you’re using insurance to cover your teletherapy sessions, here’s what you need to know about how billing works and how it may be updated based on your insurance provider’s processing.
How Insurance Billing Works
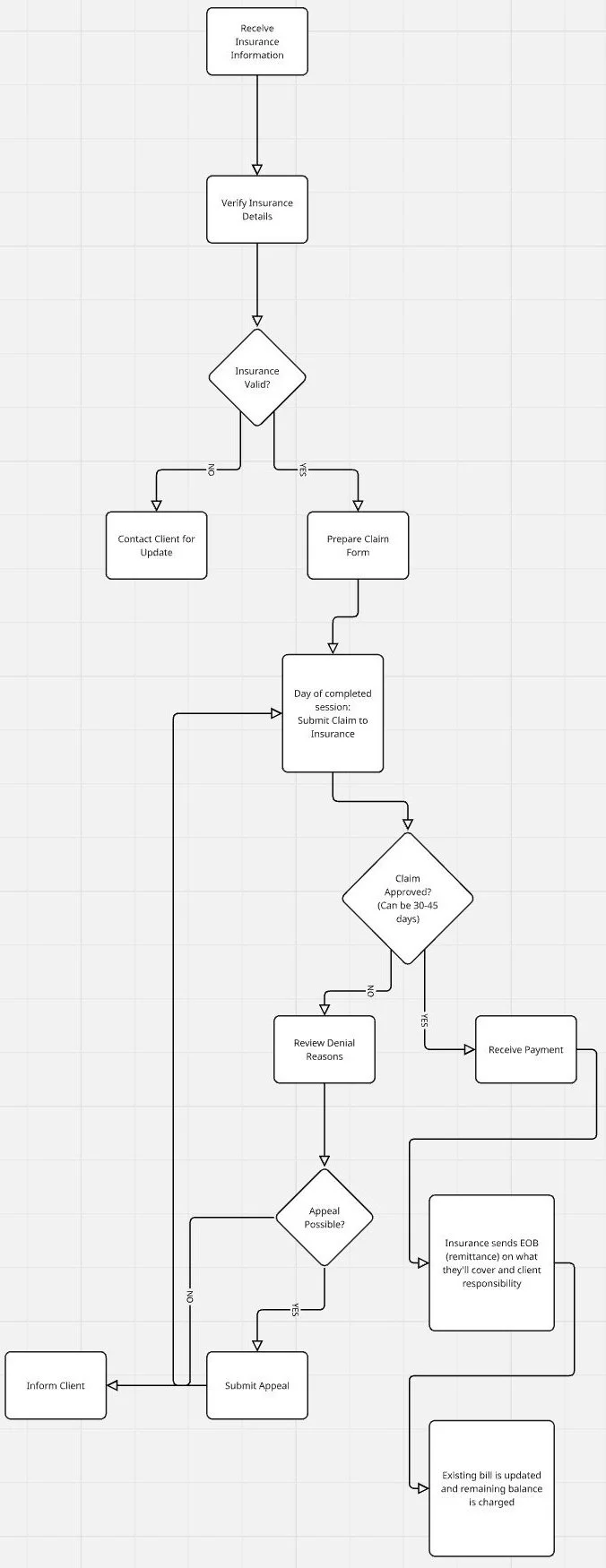
Initial Billing: After your session, we submit a claim to your insurance company based on the information available at the time of your appointment. Since payment is due at the date of service, practice clients are automatically charged on that date and also if there’s a pending balance after insurance processes a claim that is not paid by insurance.
Insurance Processing: Your insurance provider reviews the claim and determines the amount they will cover based on your plan’s benefits, deductible, co-pay, or co-insurance. Processing time can take from 30-45 days or longer depending on your insurance.
Remittance Report & Adjustments: Once we receive the Explanation of Benefits (EOB) or remittance report from your insurance company, there may be updates to your bill based on what they have approved, denied, or adjusted.
Why Your Bill May Be Updated Later
Insurance Adjustments: If your insurance provider applies a different rate or denies part of the claim, we may need to update your balance accordingly.
Deductibles & Co-Pays: If your deductible has not been met or if your co-pay differs from what was initially estimated, adjustments may be necessary.
Co-Insurance Updates: In some cases, you may not be charged co-insurance initially until we receive the remittance report from your insurance provider, at which point your bill may be updated to reflect the correct amount.
Corrections & Appeals: If there are errors or if an appeal is needed, adjustments may be made after further communication with your insurance provider.
Credit Reimbursement: At the end of the month, we check if there’s a credit on your account. This can happen due to the amount of co-insurance changing if you had a shorter session. We’ll typically refund any credit we have on your account at the end of the month or adjust your account as needed (for example, if you’ve met your deductible).
What This Means for You
You receive an initial statement that has your copay/co-insurance cost (note: co-insurance may not be charged until we get your first EOB, and then subsequently charged) and the amount we are charging your insurance. Note, this initial statement does not reflect the final amount that insurance decides to cover, but what is sent to insurance initially.
If your insurance denies a claim or does not cover the full amount, you may be responsible for the remaining balance.
If the amount your insurance doesn’t cover causes financial hardship, we can support by working with you to create payment plan/schedule options.
If you believe your insurance made a mistake, you’ll need to call them to discuss this and let us know so we can follow up with them too. Tip: When you your insurance, ask for the name of the representative, date/time of the call and ask for the reference number for the call.
Need Help?
Our billing team is here to assist you! If you have questions about your bill, insurance coverage, or payment options, please reach out to us through our Contact Us page. We want to ensure that you fully understand your billing and can focus on your therapy journey with peace of mind.
Insurance Billing and Medicaid (Apple Health)
Medicaid—also known as Apple Health in Washington State—is a government-funded insurance program that provides health coverage for eligible clients. When someone uses Medicaid (Apple Health) for teletherapy, the program typically covers the cost of virtual mental health services, just as it would for in-person therapy, as long as the provider is approved by Medicaid (Apple Health). Clients usually don't have to pay out of pocket, though this can vary slightly by state.
We ask all clients to have a credit card on file and must adhere to the attendance policy to ensure continuity of care and avoid disruptions in service. We bill Medicaid (Apple Health) through your Managed Care Organization (MCO) which are insurances that work with Medicaid, and care is provided through a secure video platform, making therapy more accessible for many individuals. Should your Medicaid (Apple Health) services end, we would then need to update your information to your new insurance or plan for self-pay/private pay.
Instructions for Clients Calling Their Insurance for Mental Health Teletherapy Coverage
When calling your insurance company to check your teletherapy (online therapy) benefits, have your insurance card, a pen, and paper ready to take notes. Here’s what to ask:
1. General Teletherapy Coverage
“Does my plan cover telehealth or teletherapy for mental health services?”
“Are virtual therapy sessions covered the same as in-person sessions?”
“Do I need to use a specific telehealth platform or provider?”
“Is my mental health benefits through the same insurance company as my medical benefit, or ‘carved out’ to a different insurance company?”
2. Costs & Payment Details
“What is my deductible, and how much of it has been met?”
“What is my copay or coinsurance for teletherapy sessions?”
“What is my out-of-pocket maximum?”
3. Provider & Preauthorization Requirements
“Do I need to see an in-network provider, or do I have out-of-network benefits?”
“Do I need preauthorization before starting teletherapy?”
“Is there a limit on the number of teletherapy sessions covered per year?”
Therapists have different licenses, and insurance plans may have specific requirements. Ask:
“Does my plan cover teletherapy provided by the following licensed professionals?”
Psychologists (PhD, PsyD)
Licensed Clinical Social Workers (LCSW, LICSW)
Licensed Professional Counselors (LPC, LPCC, LMHC)
Licensed Marriage and Family Therapists (LMFT)
Psychiatrists (MD, DO) for therapy, not just medication management
“Does my plan cover sessions with associate-level therapists (e.g., Associate Clinical Social Worker [ASW], Associate Marriage and Family Therapist [AMFT], Associate Professional Clinical Counselor [APCC]) who are working under supervision?”
“Are there any restrictions based on the therapist’s license or credentials?”
“Does the therapist need to be licensed in my state for reimbursement?”
4. CPT Codes for Teletherapy (Ask if These Are Covered)
These are common Current Procedural Terminology (CPT) codes used for teletherapy:
90791 – Initial diagnostic evaluation
90834 – Individual therapy, 45 minutes
90837 – Individual therapy, 60 minutes
90847 – Couples or family therapy with patient present
90846 – Family therapy without patient present
98966-98968 – Telephone therapy (if applicable)
Modifier 95 or GT – May be required to indicate a telehealth service
Ask the representative these questions:
“Are the above CPT codes covered for telehealth visits?”
“Do I need a specific modifier (95 or GT) on the claim for teletherapy reimbursement?”
5. Out-of-Network Coverage (If Needed)
“If I see an out-of-network therapist for teletherapy, how much will be reimbursed?”
“What is the process for submitting claims for reimbursement?”
6. Claim & Billing Questions
“If my therapist does not bill insurance directly, what is the process for filing claims?”
“Where can I find the claim form, and how long do I have to submit it?”
7. Additional Coverage Details
“Are phone-only therapy sessions covered?”
“Are there any restrictions on teletherapy, such as requiring video sessions instead of phone calls?”
“Are there any restrictions on which states the therapist can be licensed in?”
Final Step: Take Notes
Write down:
The name of the representative you spoke with
The date/time of your call
Ask for the reference numbers for the call that they provide
Instructions for Out-of-Network Mental Health Teletherapy Clients Calling Their Insurance
If you are seeing an out-of-network therapist for teletherapy, you may need to submit claims for reimbursement. Before starting therapy, call your insurance company to verify your benefits. Have your insurance card, a pen, and paper ready to take notes.
1. Verify Out-of-Network Mental Health Teletherapy Coverage
“Do I have out-of-network benefits for mental health teletherapy sessions?”
“Are out-of-network virtual therapy sessions covered the same as in-person sessions?”
“Do I need to use a specific telehealth platform for coverage?”
2. Reimbursement Rates & Costs
“What percentage of the session fee will be reimbursed for out-of-network therapy?”
“Is reimbursement based on usual and customary rates (UCR) or a set fee schedule?”
“What is my out-of-network deductible, and how much has been met?”
“What is my out-of-pocket maximum for out-of-network services?”
“Is there a limit on the number of reimbursable teletherapy sessions per year?”
3. Check If Certain Therapist Licenses & Associate-Level Providers Are Covered
Therapists have different licenses, and insurance plans may have specific requirements. Ask:
“Does my plan cover teletherapy provided by the following licensed professionals?”
Psychologists (PhD, PsyD)
Licensed Clinical Social Workers (LCSW, LICSW)
Licensed Professional Counselors (LPC, LPCC, LMHC)
Licensed Marriage and Family Therapists (LMFT)
Psychiatrists (MD, DO) for therapy, not just medication management
“Does my plan cover sessions with associate-level therapists (e.g., Associate Clinical Social Worker [ASW], Associate Marriage and Family Therapist [AMFT], Associate Professional Clinical Counselor [APCC]) who are working under supervision?”
“Are there any restrictions based on the therapist’s license or credentials?”
“Does the therapist need to be licensed in my state for reimbursement?”
4. Required CPT Codes & Modifiers
Ask if your plan covers these Common Procedural Terminology (CPT) codes for teletherapy:
90791 – Initial diagnostic evaluation
90834 – Individual therapy, 45 minutes
90837 – Individual therapy, 60 minutes
90847 – Couples or family therapy (with patient present)
90846 – Family therapy (without patient present)
98966-98968 – Telephone therapy (if applicable)
Modifiers: Ask if they require Modifier 95 or GT to indicate a telehealth service.
Example question:
“Does my plan reimburse for teletherapy sessions billed under CPT code 90837 (60-minute session) with modifier 95?”
5. Claim Submission Process
“What is the process for submitting claims for out-of-network reimbursement?”
“Where can I find the claim form?”
“What documentation is required (e.g., superbill, diagnosis code, provider information)?”
“How long do I have to submit a claim after a session?”
“How will I receive reimbursement (check, direct deposit, etc.)?”
“How long does it take for claims to be processed?”
6. Additional Coverage Considerations
“Are phone-only therapy sessions covered, or do sessions require video?”
“Are there any restrictions on which states the therapist can be licensed in?”
7. Final Step: Take Notes
Write down:
The name of the representative you spoke with
The date/time of your call
Any reference numbers for the call
The details of coverage, reimbursement rates, and provider requirements
Medical Insurance Definitions
Premium – The amount you pay for your health insurance every month.
Deductible – The amount you must pay out of pocket before your insurance starts covering costs.
Copayment (Copay) – A fixed amount you pay for a medical service (e.g., $20 for a doctor visit).
Coinsurance – The percentage of costs you pay after meeting your deductible. For example, if your coinsurance is 20%, you pay 20% of the bill, and insurance covers the remaining 80%.
Out-of-Pocket Maximum – The most you have to pay in a year before insurance covers 100% of costs.
Network – The group of doctors, hospitals, and providers that work with your insurance plan.
Out-of-Network Provider – A healthcare provider who does not have a contract with your insurance company, which may result in higher costs or limited coverage for services.
HMO (Health Maintenance Organization) – A type of plan that requires you to use in-network doctors and get referrals for specialists.
PPO (Preferred Provider Organization) – A type of plan that allows you to see any doctor but offers lower costs for in-network providers.
Preauthorization – Approval from your insurance before certain treatments or medications are covered.
Explanation of Benefits (EOB) – A remittance statement from your insurer detailing what was covered and what you owe.
Claim – A request for payment that you or your healthcare provider submit to your insurance company after receiving medical services.
Usual and Customary Rates (UCR) – The standard amount an insurance company considers reasonable for a medical service based on local rates. If a provider charges more than the UCR, you may have to pay the difference.
Set Fee Schedule – A fixed list of prices that an insurance company agrees to pay for specific medical services, regardless of the provider’s actual charges.
Superbill – A detailed receipt from a healthcare provider that includes services, fees, and necessary insurance codes, used by patients to submit claims for out-of-network reimbursement.
